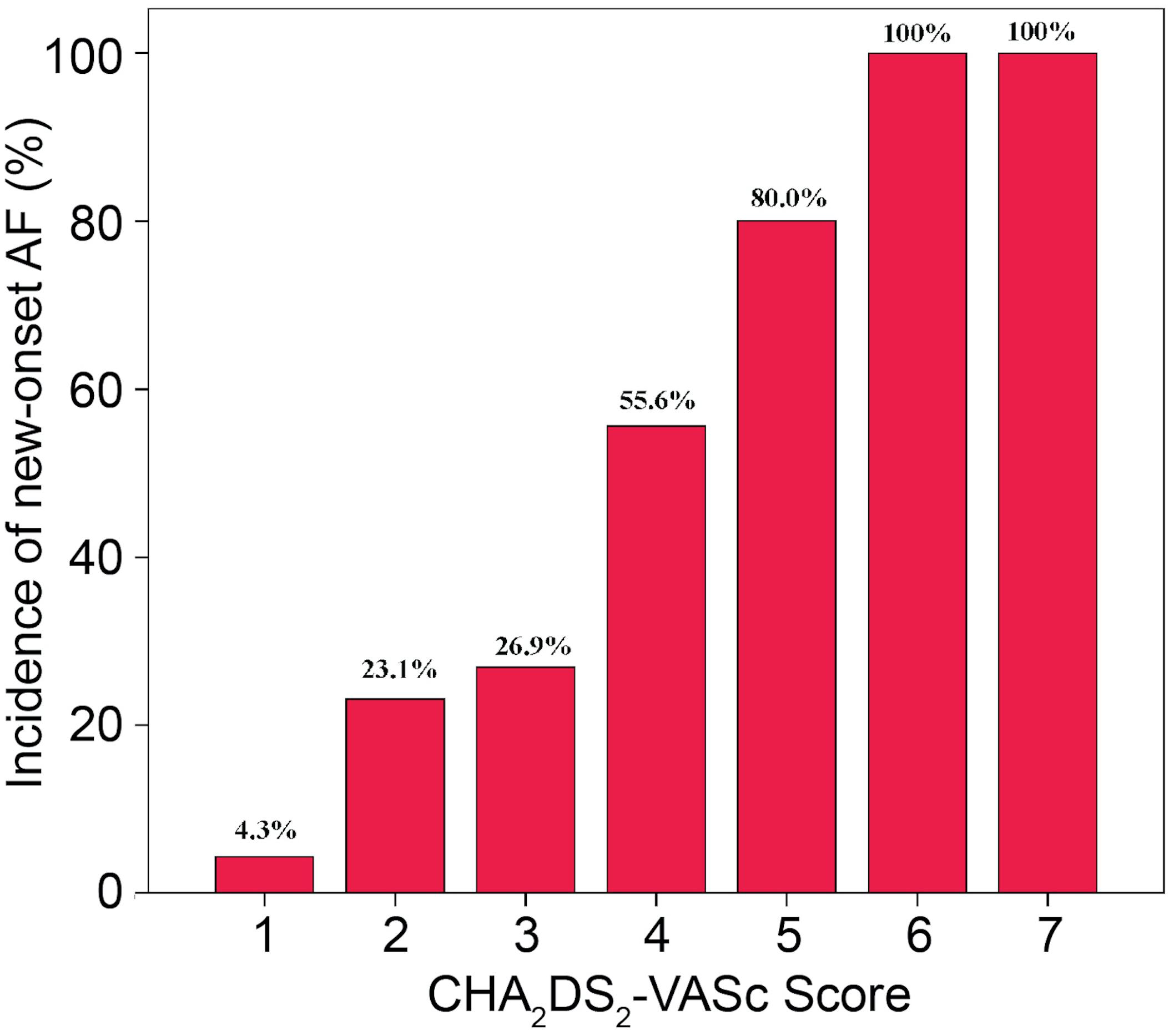
8 However, the main issue is the high rate of atrial tachyarrhythmias (ATAs) following the catheter ablation procedure. In AF patients with left ventricular ejection fraction (LVEF) ≤35%, catheter ablation gives additional benefit in reducing hospitalisation due to worsening heart failure and all-cause mortality. 5 Compared with antiarrhythmic drugs (AADs), catheter ablation significantly reduces the AF recurrence rate, provides better symptom control and improves the quality of life in AF patients. 4Ĭomplete PV isolation (PVI) by single-shot or point-by-point catheter ablation approach is the cornerstone of catheter ablation in AF patients. 3 In contrast, AF induced by pacing protocol during typical AFL ablation is a strong predictor for AF. 2 Pulmonary vein (PV) firing during AF episodes makes an essential contribution to initiating typical AFL. 1 The presence of AFL is documented in 20.6% of AF patients. Conclusion: This study suggested that prophylactic CTI ablation was an ineffective and inefficient approach in AF without documented typical atrial flutter patients.ĪF and atrial flutter (AFL) commonly coexist, and reveal a strong clinical interrelationship. Additional prophylactic CTI ablation to pulmonary vein isolation significantly increased the radio frequency application time (standardised mean difference 0.52 95% CI p=0.03). 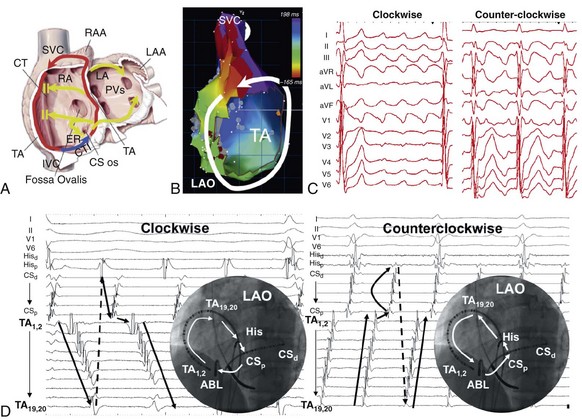
Prophylactic CTI ablation was associated with a higher recurrent AF rate (33.8% versus 27.1% risk difference 0.07 95% CI p=0.02). The risk of atrial tachyarrhythmias following a successful catheter ablation procedure was greater in the pulmonary vein isolation + CTI ablation group than pulmonary vein isolation alone group (34.8% versus 28.2% risk difference 0.08 95% CI p=0.04). Results: A total of 1,476 patients from four studies were included. The pooled effects were presented as the risk difference and standardised mean difference for dichotomous and continuous outcomes, respectively. The overall effects estimation was conducted using random effects models. Methods: A systematic review and meta-analysis study was conducted. The present study aimed to evaluate the role of prophylactic CTI ablation in this population. Based on these results, the conventional waiting period is unnecessary in 97.6% patients without dormant conduction after CTI-dependent flutter ablation.Īdenosine atrial flutter catheter ablation cavitricuspid ablation reconnection.Background: The advantage of prophylactic cavotricuspid isthmus (CTI) ablation for AF patients without documented atrial flutter is still unclear. All 4 patients underwent further ablation.Ī negative adenosine challenge immediately after CTI ablation with bidirectional block, or after abolition of dormant conduction with further ablation, strongly predicted the absence of subsequent spontaneous reconnection within 30 minutes. Two other patients (1.2%) developed late dormant conduction with adenosine at 30 minutes. Two patients (1.2%) had subsequent spontaneous time-dependent reconnection within 30 minutes. Nine patients (5.3%) had dormant conduction across the CTI immediately after ablation and BDB, and required further ablation. After the achievement of BDB without dormant conduction, spontaneous CTI reconnection during the following 30 minutes and dormant conduction with adenosine at 30 minutes were evaluated.Ī CTI block was achieved in 171 patients. In cases of dormant conduction, the CTI was ablated again until its abolition. Following the completion of CTI ablation and documentation of BDB, adenosine (≥12 mg IV) was administered immediately. Conventional practice involves a waiting period of 20 to 30 minutes after achievement of a bidirectional line of block (BDB) to monitor for recovery of conduction.Īssess whether abolition of dormant conduction with adenosine immediately after CTI ablation and BDB can predict the lack of CTI conduction recovery during the following 30 minutes.Ĭonsecutive patients undergoing catheter ablation for CTI-dependent atrial flutter were studied. Dormant conduction unmasked by adenosine predicts clinical recurrences of cavotricuspid isthmus (CTI) dependent atrial flutter following catheter ablation.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |

 RSS Feed
RSS Feed
